If your hip is damaged by arthritis, a fracture, or other conditions, you may experience a progressive intense pain along with difficulty in daily functions like walking or climbing stairs. In some cases, you may experience pain even while resting. The cartilages in the hip joint can be damaged particularly in conditions like arthritis, whose progression is almost inevitable. In such severe conditions, surgical treatment option known as hip replacement surgery is used to control the hip joint damage.
What is hip replacement surgery?
Hip replacement is a surgical procedure where the damaged sections of hip joint is removed and replaced with artificial implants. The procedure aims to relieve pain, increase motion and help you get back to your normal activities. Hip replacement surgery is a safe and effective procedure. Total hip replacement is also referred to as total hip arthroplasty.
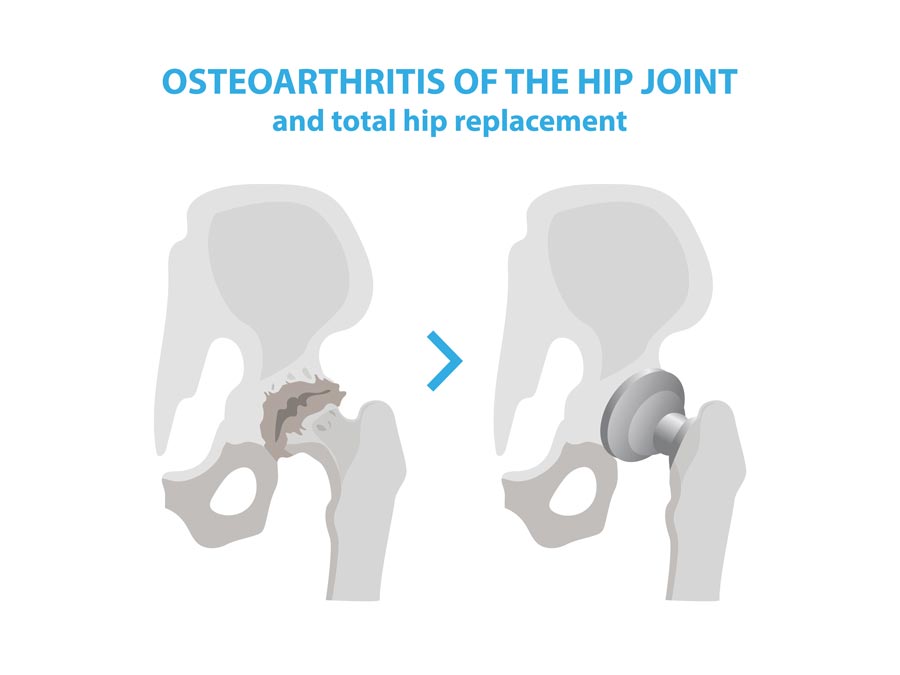
When is hip replacement surgery recommended?
Hip replacement surgery is usually recommended when the hip joint is worn or damaged by conditions like:
- Osteoarthritis: It occurs when the protective cartilage, which cushions the ends of your bones, damages over time. It is the most common reason for hip replacement surgery.
- Rheumatoid arthritis: It is a progressive autoimmune disease that causes pain and damage in the joints of our body.
- Osteonecrosis: It is the condition characterized by the death of bone tissue due to lack of blood supply. When the blood supply to the femoral head is limited because of any injury to the hip, it will cause the bone surface to collapse leading to arthritis.
- Hip fractures: A hip injury or fracture will damage the cartilage of the hip causing pain and stiffness over time.
Apart from all these causes, disorders like bone dysplasia that leads to unusual bone growth, may also lead to hip replacement surgery.
A hip replacement surgery is recommended if:
- You have hip pain that persists despite medications and interferes with your daily activities.
- You have limited ability to move or lift the leg due the stiffness in the hip.
- Your symptoms are not adequately alleviated by non-surgical treatments.
What are the pre-procedure steps?
Once your surgeon recommends hip replacement surgery as the best method to relieve pain and increase the mobility of your hip joint, few steps have to be followed before undergoing surgery to improve the results and also to avoid complications related to the surgery. The pre-procedure steps include:
- Physical examination: Your orthopedic surgeon will refer you to a general physician for a complete physical examination. This is to make sure that you are healthy enough to undergo the surgery. Any indications of infections or diseases of heart, lungs or uncontrolled diabetes will postpone total hip joint surgery.
- Laboratory tests: In addition to the general medical examination, your doctor may ask you to undergo some diagnostic tests like blood and urine tests, an electrocardiogram (EKG), and chest x-rays, which help to plan your surgery.
- Lifestyle modification:
- You may be asked to lose some weight before surgery (a goal body mass index [BMI] of less than 40) to minimize the stress on your new hip and other possible complications after the surgery.
- If you have a habit of smoking, your surgeon will ask you to stop smoking before your surgery as smoking can delay wound healing and slow down the recovery period. You may be asked to quit smoking a month before surgery and for at least two months after surgery.
- You may be referred to a physiotherapist, who will guide with some conditioning exercises to strengthen the muscles and increase the flexibility.
- You may be asked to lose some weight before surgery (a goal body mass index [BMI] of less than 40) to minimize the stress on your new hip and other possible complications after the surgery.
- Medications: Your orthopedic surgeon will enquire about the medications you are taking and may advise you to stop taking some medicines which may interfere with the surgical procedure. E.g. Aspirin is often discontinued one week prior to surgery as it may increase the risk of bleeding during the surgery.
- Dental checkups: You are advised not to have any dental procedures including teeth cleaning, several weeks before surgery and after surgery. There is a chance for bacteria to enter the bloodstream during dental procedures, which can cause hip infections after the surgery.
- Blood Donations: The surgery can involve blood loss, so you may be advised to donate your own blood prior to surgery. This will help in minimizing the risks related to blood transfusions.
- Social and home planning: Your healthcare team will advise you to make necessary arrangements prior to the surgery, such as to have someone to drive you back home and to assist you at home during the recovery period after surgery.
How is hip replacement surgery performed?
Hip replacement usually requires a hospital stay where you will be admitted to the hospital on the day of your surgery.
Hip replacement surgery is done under anesthesia. Once you are admitted for the surgery, the anesthesia team will evaluate your health status and will check whether you are allergic to any anesthetic medications. You will be given either general anesthesia (which puts you to sleep during the procedure) or spinal anesthesia (which makes your body numb from the waist down), depending on your condition and procedure.
The general steps involved in a hip replacement surgery are as follows:
- Before the surgery begins, you will be asked to wear the surgical gown and then will be moved to the operation room.
- You will be positioned in the operation table and the anesthesiologist will administer the anesthetic. The anesthesia team will monitor your heart rate, blood pressure, pulses, and oxygen level during the surgery.
- To begin, surgeon will make an incision over the front or side of your hip. The damaged parts are then carefully removed. It is then replaced with prosthesis made of metal, plastic, or ceramics.
The hip prosthesis consists of a metal or ceramic ball that replaces the round head of the thigh bone (femur), with the stem inserted into the thigh bone and a bowl-shaped part which replaces the socket in the pelvis. - The prosthesis is shaped accordingly and is placed in the right place.
- The surgeon will check the joint for ease of movement, its position and restoration of the proper anatomy of the hip, including leg length.
- X-rays are taken to assure proper sizing and positioning of the implant.
- The incision is closed with stitches or surgical staples and bandages are applied on the site.
What are the post-procedure care?
You will be moved to the recovery room after the surgery and will be monitored until you recover from anesthesia. Once you wake up, you will be taken to your hospital room. In most cases, you will be admitted in the hospital for one or two nights.
Hospital care: The hospital team will try to get you walking as soon as possible, often the same day after the surgery. A physical therapist will meet you after your surgery and will plan an exercise rehabilitation program for both, hospital stay and after being discharged.
Intravenous fluids are administered to maintain the electrolyte levels and to replace any fluids lost during surgery. Along with IV fluids, antibiotics as well as pain medication is also administered.
After the surgery there will be an increased risk of blood clots in your legs. You will also be administered with anti-coagulants to prevent those blood clots.
In some cases, patients may have trouble with urination. Catheters are placed into the bladder to allow normal passage of urine.
At home:
Once you're ready to be discharged, orthopedic surgeon will give instructions regarding home care during the first few weeks after surgery which includes:
- You'll need to use frame or crutches for one or two weeks after the surgery.
- You must keep the surgical area clean and dry to prevent infections and irritation from the surgical dressings.
- A diet rich in iron will promote proper tissue healing and restore muscle strength. It is also important to drink plenty of fluids.
- Exercise is the vital component for a speedy recovery. Follow your physiotherapist’s instructions and do exercises that will restore movement and strengthen your hip muscles.
- As rehabilitation progresses (3 to 6 weeks following surgery), you may be able to do less-strenuous regular activities.
- 6 to 12 weeks after surgery, you'll have a follow-up with your surgeon to examine the healing pattern of the hip. Based on the diagnosis, you will be able to return to an active lifestyle.
Outlook
Hip joint replacement surgery is one of the safest and most successful joint surgeries performed. It provides a complete symptomatic relief of arthritic hip pain. Duration required for healing and rehabilitation varies among patients. A successful treatment can be achieved when the patient, physical therapist, and doctor work together. After the surgery most patients will experience a better range of motion, less pain and stability. The artificial implants usually last longer, however a high impact activity or obesity may affect its lifespan. A second hip replacement is also possible if the first implant deteriorates.
With newer devices and technologies, total hip surgery will further improve patient outcomes, mobility, and lessen the complications of traditional surgery.
Sources
- Total Hip Replacement. https://orthoinfo.aaos.org/en/treatment/total-hip-replacement/. Accessed on: 12-03-2020.
- Hip replacement. https://www.mayoclinic.org/tests-procedures/hip-replacement/about/pac-20385042. Accessed on: 12-03-2020.
- Hip Replacement Surgery. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/hip-replacement-surgery. Accessed on: 12-03-2020.
- Hip replacement. https://www.nhs.uk/conditions/hip-replacement/. Accessed on: 12-03-2020.



